BCAN-RAY
A study looking at improving the risk assessment of breast cancer in younger women
Breast cancer
Breast cancer is the leading cause of death in women aged 35-50 years in the UK, with an estimated 10,000 women a year diagnosed under the age of 50. Currently, two approaches are used in the UK to screen women for breast cancer:
- Based on age, with all women invited to breast screening every three years from the age of 50
- Based on family history, with women who are known to have a of breast cancer (where breast cancer is diagnosed in multiple family members and/or at younger ages) being invited for breast screening before age 50. This can sometimes be from as early as 25 years for those at highest risk but is more commonly from age 40
Breast cancer risk is also impacted by other factors such as the age which a woman’s periods start and stop, the age at her first pregnancy and number of subsequent pregnancies, whether a woman breast feeds, obesity and the density of the breasts on a mammogram.
An analysis of the genetic makeup can identify those at higher risk using a tool called a polygenic risk score. This can be derived from a saliva sample and is a powerful predictor of breast cancer risk.
The BCAN-RAY study
There is a large cohort of women between 30-50 who are at risk from breast cancer before they are eligible for screening. However, current risk assessments within this age group are limited to women with a family history of breast cancer. Only about 5% of women have a strong enough family history of breast cancer to be eligible for such screening and more than two thirds of women who develop breast cancer, even at a young age, do not have any family history of the disease.
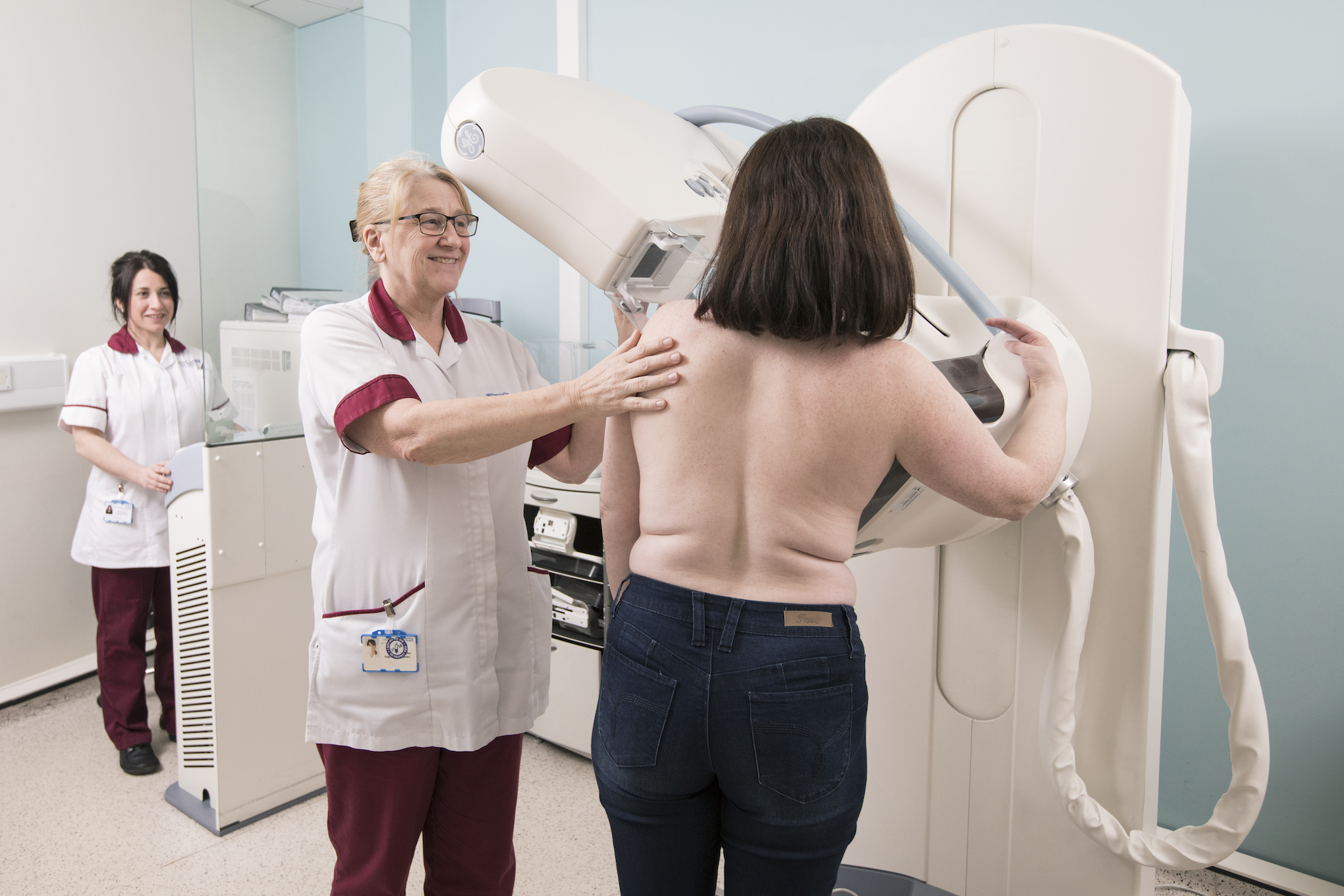
The Breast CANcer Risk Assessment in Younger women (BCAN-RAY) study began in May 2023, and is a comprehensive breast cancer risk assessment strategy for women aged 30-39 years. It incorporates a questionnaire of breast cancer risk factors, assesses breast density through a low-dose mammogram (which uses less than 10% of the radiation dose of a standard mammogram) and a saliva sample assessing the polygenic risk score.
The BCAN-RAY study, led by Manchester University NHS Foundation Trust (MFT) involves recruiting 1,000 women aged between 30 and 39 years old from across Greater Manchester and East/Central Cheshire.
250 women (case participants) previously diagnosed with breast cancer without a strong family history of the disease will be studied alongside 750 women (control participants) in the same age group who have not had breast cancer, and who also have no strong family history of the disease. Control participants will be recruited through participating GP surgeries and will be seen at the Nightingale Centre at Wythenshawe Hospital, part of MFT. Case participants will take part in the study at breast oncology centres across Greater Manchester and Cheshire – including The Nightingale Centre and The Christie hospital.
Control participants undergo a low-dose mammogram to assess the density of their breasts and provide saliva samples to look at their DNA in addition to completing self-report questionnaires. Additional questionnaires will evaluate additional psychological factors, including potential harms such as heightened state anxiety and breast cancer specific worry, and the level of satisfaction regarding their decision to participate. Participants may also report potential benefits, such as feeling more knowledgeable about breast cancer risk.
Additionally, a subset of approximately 24 women, evenly split between those at average risk and those at increased risk, will participate in semi structured interviews. These interviews aim to gauge the acceptability of the risk assessment strategy and pinpoint any necessary modifications to enhance its uptake.
Researchers will also compare the uptake rates to the study by socioeconomic status and ethnicity between those who participate in the study and those who decline participation.
Aims of the BCAN-RAY study
The BCAN-RAY study aims to evaluate a comprehensive breast cancer risk assessment strategy among a diverse ethnic and socioeconomic population of women aged 30–39 years without a strong family history of breast cancer.
This study aims to find out:
- How strong a risk factor dense breast tissue is for young women
- How to include this when working out their risk of breast cancer
- The potential harms and benefits of participating in breast cancer risk assessment
- How to maximise the acceptability of breast cancer risk assessment among young women
The pioneering study launched in memory of Girls Aloud singer, Sarah Harding and is one of the first research studies in the world to identify new ways to predict the risk of younger women getting breast cancer.
BCAN-RAY live-lounge with Dr Sacha Howell and Dr Sarah Hindmarch
BCAN-RAY Chief Investigator, Dr Sacha Howell, Senior Lecturer at The University of Manchester and Honorary Consultant in Medical Oncology at The Christie hospital and MFT, discusses the study alongside Dr Sarah Hindmarch, Research Associate (Cancer Early Detection) at The University of Manchester. Watch this 9 min 38 sec video on the MCRC YouTube channel.
BCAN-RAY contributors
Dr Lorna McCune
GP Partner and Research Lead from St John’s medical centre
“We at St John’s, have been thrilled to be a part of this study. It is important to make a difference to young people who are at increased risk of breast cancer in the future. As there is no screening program yet on a national level for this group, we were really pleased to be able to offer this opportunity to our patients. Currently there have been 54 participants from St John’s that have been given their risk feedback, 37 of these were found to be at average risk and 17 were found to be at increased risk and will therefore be able to access to early screening and preventative treatment. Sarah’s legacy has made this possible, and it has been wonderful to work alongside Dr Sacha Howell and his team who were really supportive to us as the first GP site to refer patients to the study.”

Professor Sue Astley
Co-investigator on Mammographic density from The University of Manchester
“One of the novel aspects of BCAN-RAY is the use of mammograms that are taken with only about a tenth of the usual X-ray dose and analysed with Artificial Intelligence (AI). We have developed a state-of-the art AI algorithm to estimate mammographic density from the low dose images. This is important because high breast density is known to be associated with an increased risk of developing breast cancer.”

Eleanor Roberts
University of Manchester ACED PhD Student, Manchester Foundation Trust
Eleanor’s main role is in the Pathogenic Variant result and PRS for the breast cancer risk feedback.
“I work on the genetic aspect of the study, processing all the saliva samples. I extract the DNA and analyse the genetic results to see whether the participants have a gene alteration that increases their lifetime risk of developing breast cancer. I also help with the processing of the polygenic risk score (PRS), a personalised risk score predicting each individual’s risk of developing breast cancer.
My work in this study is important as genetic risk is a keystone in personalised risk prediction. If we detect a genetic alteration in a breast cancer risk gene or calculate a high PRS, this woman could then make informed decisions about her health to reduce her risk of breast cancer or detect it at a much earlier and more treatable stage. I feel incredibly proud to be a part of this vital research determining risks of breast cancer in young women and hope that one day this can be implemented on a national scale.”

Jake Southworth
Clinical Trials Administrator from Manchester Foundation Trust
Jake’s main role is in the co-ordination and administration of the study.
“I started my career in research when I was 19, and my interest in both research and on prevention and early detection (PED) studies have grown since then, especially since both my mother and aunt were diagnosed with breast cancer recently and so I have both a professional and personal interest in the area. Working on the BCAN-RAY study is important as we are able to identify those at higher risk of developing breast cancer and start them on earlier preventions which can increase survivability if they were to ever be diagnosed. I am proud to be working on this important study and really enjoy working with the team.”

Helen Ruane
Senior Clinical Research Practitioner from Manchester Foundation Trust
Helen’s main role is the recruitment of participants who have not been diagnosed with breast cancer (control group) and conducting their research study clinic appointments (e.g. checking eligibility; explaining details of the study; answering questions; receiving informed consent; supporting participants to complete their breast cancer risk factor questionnaire and psychological wellbeing questionnaires; facilitating the collection of saliva samples and assisting to organise and enabling their low dose mammograms to be performed).
“I’ve always had an interest in research studies which focus on prevention and early detection (PED) especially since a close relative was diagnosed with breast cancer at a young age. A strong motivation for working on the BCAN-RAY study was appreciating the importance of early detection of cancer because treatments are more likely to be successful if diagnosed at an early stage. I really enjoy working on this important study especially meeting the participants who give so generously of their time to take part.”

Next steps
The BCAN-RAY study should complete recruitment in May 2025 and results will be then analysed and presented. If the approach is deemed to be successful, acceptable to women and potentially cost-effective for the NHS funding will be sought to run a larger study across Greater Manchester.
Current Media coverage
- Dr Howell featured live on ITV Granada Reports in June 2023 alongside the first participant, Catherine Craven-Howe.
- In August 2023, BBC Morning Live filmed at The Nightingale Centre, part of MFT as part of a seven-minute film, led by Girls Aloud bandmate, Kimberley Walsh. You can watch this film on the BBC website here.
- In September 2023, the study was featured on Good Morning Britain and ITV Granada Reports. This included headline news mentions every hour, a short news package featuring an interview clip from Dr Sacha Howell and a study participant, and a 10-minute interview with Nicola Roberts (Girls Aloud bandmate) and Dr Hilary(GP who regularly features on the show) to discuss the study. Further coverage includes: ITV News, Daily Mail, Manchester Evening News, The Independent, The Mirror, Evening Standard and more.
- In May 2024, Dr Sacha Howell featured on Sky News alongside study participant, Anna Housley, who found she was at ‘increased risk’ of developing breast cancer after taking part in the study at The Nightingale Centre. Further coverage includes: BBC Radio Manchester, Capital Radio, BBC News, The Mirror (also in print), Sky News, Manchester Evening News, Hits Radio and more.
Funders
The BCAN-RAY study is led by Manchester University NHS Foundation Trust, delivered at The Nightingale Centre at Wythenshawe Hospital and breast oncology centres across Greater Manchester and Cheshire.
The study is funded by Cancer Research UK via the International Alliance for Cancer Early Detection (ACED), The Christie Charity and The Shine Bright Foundation. Dr Sarah Hindmarch’s PhD was funded by the Manchester Cancer Research Centre.
Helpful links
- CRUK: A study looking at improving the risk assessment of breast cancer in young women (BCAN-RAY)
- Feasibility and acceptability of offering breast cancer risk assessment to general population women aged 30-39 years: a mixed-methods study protocol
- https://www.christie.nhs.uk/the-christie-charity/donate/a-letter-from-girls-aloud