LAMNs and Pseudomyxoma peritonei
Building a living biobank
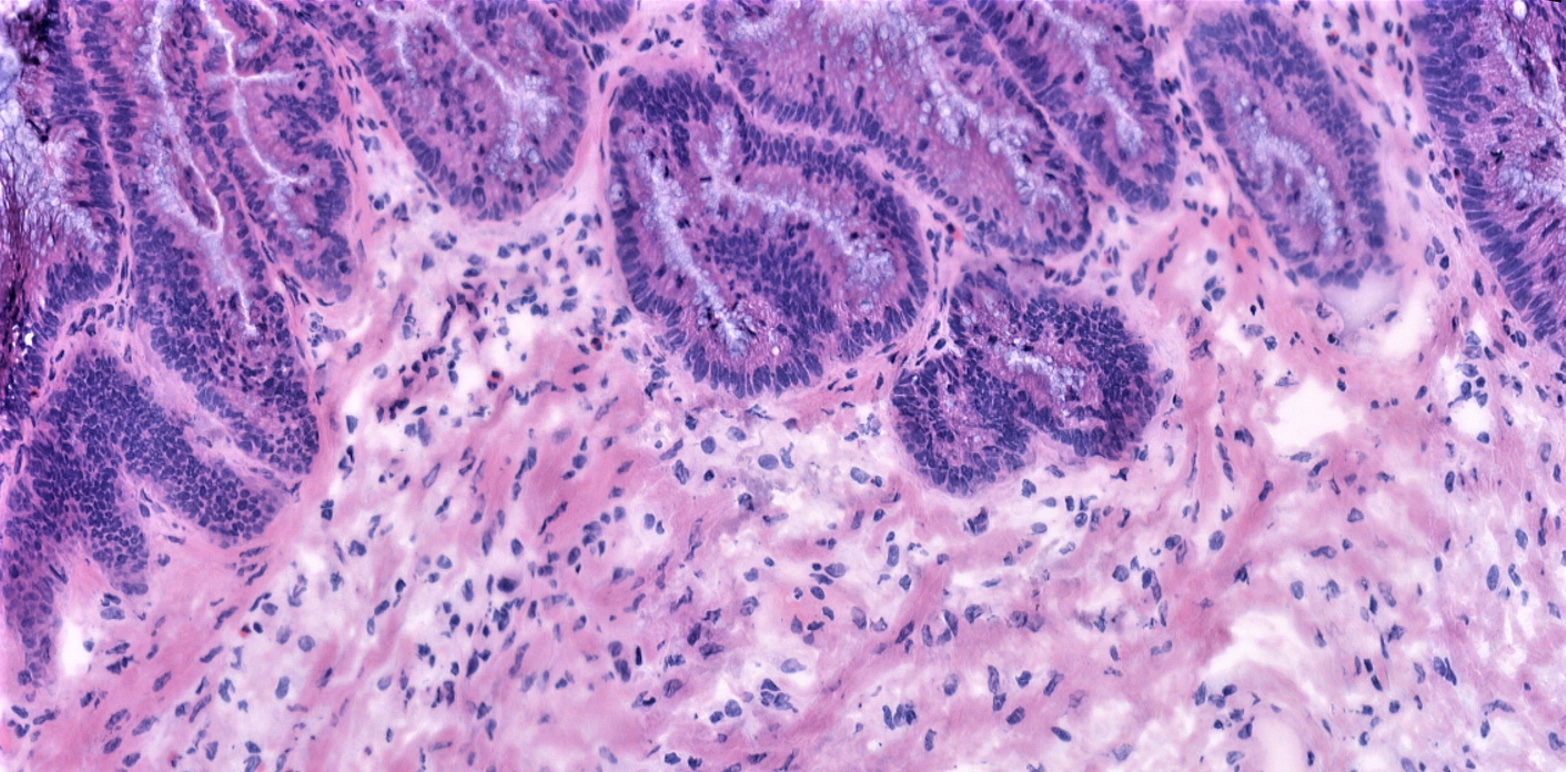
Pseudomyxoma peritonei (PMP) is a condition that arises as a result of tumour cells (metastasis) from a low-grade appendiceal mucinous neoplasm (LAMN) spreading into the abdominal (peritoneal) cavity. This causes an accumulation of a large amount of solid and liquid mucinous material causing abdominal distension, malnutrition and ultimately mortality. LAMNs are rare tumours with an estimated incidence of only 1-2 cases per million and so understanding the nature of this tumour type has proven difficult in the past due to a lack of samples.
Previously, PMP has been treated through aggressive cytoreductive surgery and hyperthermic intraperitoneal chemotherapy, but despite these interventions over 30% of cases of PMP recur. At present, there is no standard anti-cancer treatment or targeted treatment available for this rare tumour.
There are very few units in the world that have access to the number of samples for patients with LAMNs as we do in Manchester. We have some world-leading expertise in genomics, transcriptomics, cell culture, organoid development and we have a cancer centre for applied pharmacokinetic research, which means we’ve got the right experts around the right patient population.
Omer Aziz
Lead for the CPOC peritoneal tumour service and lab at the MCRC
Manchester Research
LAMNs are notoriously difficult to sample due to their slow-growing nature and an abundance of mucinous material. The MCRC Biobank team have developed world-leading protocols for collection of samples from PMP patients and were instrumental in securing a prestigious CRUK accelerator award in 2020 for PMP. These protocols are being used in four centres across the UK, Italy and Spain over the next five years to collect samples from patients with PMP allowing for genomic and transcriptomic analysis as well as cell culture and organoid development. This will help researchers to understand the nature of these tumours, why certain patients respond better to therapies than others and could help identify future treatment targets delivering more personalised cancer care.
The MCRC Biobank team, led by Jane Rogan are working with surgeons, histopathologists, oncologists and scientists at The Christie Colorectal and Peritoneal Oncology Centre (CPOC) peritoneal tumour service, CPOC Lab at the MCRC, Wellcome Trust Centre for Cell-Matrix Research at The University of Manchester, Manchester Centre for Genomic Medicine, and The University of Manchester School of Pharmacy.
We are PMP specialists with over 20 years’ experience of treating these patients. We know that the treatment options for these patients haven’t advanced at all in those 20 years and that is where this project comes in.
Omer Aziz
The importance of international collaborations
The PMP CRUK Accelerator Award study is the most comprehensive of its kind on this patient group and it has exemplified the importance of international collaborations. Due to the rarity of the cancer, colleagues from Instituto Nazionale dei Tumori di Milano in Italy, Val d’Hebron Insitute of Oncology in Spain and The University of Manchester and The Christie all need to work collaboratively. The main goal is to share knowledge and insights so that research protocols can be seamlessly integrated at each site, this includes:
- Developing the protocols that will allow the formation of a living biobank of PMP samples across the three countries
- Investigating the impact of immune and molecular signatures on long term outcome for a subset of patients with PMP
- Seeking to identify new drug targets based on genomic/transcriptomic analyses and verify any drug candidates in organoid models.
This reciprocal learning means that the team has been able to learn from the techniques adopted by their counterparts and has resulted in a reduced number of steps in developing a project of this kind.
Key challenges
This research involves vast collaboration to standardise and optimise prospective sample collection process from a notoriously challenging tumour type. Standard operating procedures have been developed and shared with the whole consortium and as a next step, samples are being quality checked for nucleic acid and sequencing library integrity to standardise RNA and DNA extraction across the three countries.
The inception of this project coincided with the beginning of the COVID-19 pandemic, in March 2020. Progress was restricted due to the closure of the MCRC Biobank limiting the opportunity to collect and analyse tumour samples. However, the team overcame many obstacles through use of technology and remote working.
The team have shown that the majority of samples that have been collected can be used for the research. However, as this is a difficult tumour type to grow the team will continue to face challenges in developing cell cultures and organoids for this living biobank.
Identifying this unmet need was a combination of the acknowledgement of the need for this research, the will of researchers to progress in this field and the CRUK accelerator providing the big opportunity for us to develop this platform on which we could do the research.
Omer Aziz
Next steps
This project will be ongoing for five years, with the hopes of collecting samples from 400 patients and create the largest biobank of its kind for LAMNs. The study will enable researchers to better predict patient outcomes based on the genes within their tumours.
“This research is going to help us understand the process of how these tumours grow, spread and live within the peritoneal cavity so that we can then target some of those processes.
“It’s also going to allow us to update the treatment options for these patients who are currently receiving 20-30-year-old drugs which are based on another tumour type. For the first time we may be able to have a treatment that is specific to this tumour not translated from another tumour,” Omer concluded.

